FEES helps Speech Language Pathologists pinpoint why patients have trouble swallowing
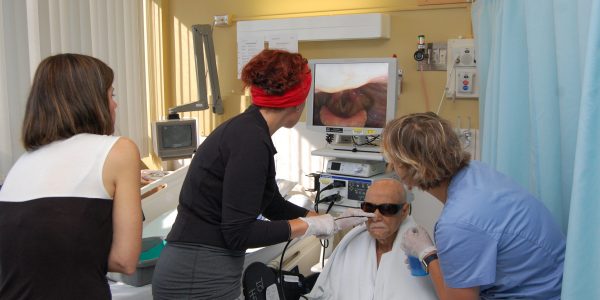
Mr. K., a 91-year-old patient on the neurology ward at Lions Gate Hospital, sits motionless as Jana Tutt, a Speech Language Pathologist (SLP), inserts an endoscope into his nose. The endoscope – a small tube with a high definition camera and light on the end – will see what’s happening inside Mr. K’s throat when he swallows.
As Jana gently guides the endoscope through his nostril and brings it to rest above his vocal cords, SLP Practice Leader Ali Duke, and FEES Trainer Cathy Silversides, closely watch the monitor and offer Mr. K small sips of water, dyed blue with food colouring.
When Mr. K was admitted to LGH following a stroke, Jana assessed his swallowing at bedside, looking for clinical signs that food and fluid might be entering his airway (“aspiration”), putting him at risk for pneumonia.
Procedure possible thanks to LGH Foundation donation
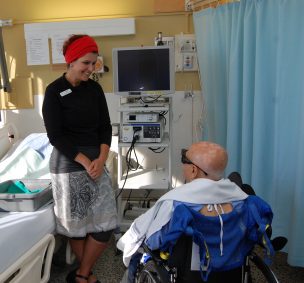
Speech Language Pathologist Jana Tutt reviews the information with the patient following the FEES procedure.
Wanting to investigate his swallowing function further, she requested that his doctor order a FEES (Fiberoptic Endoscopic Evaluation of Swallow). The procedure, pioneered in the 1980s by SLPs and widely used across North America, has been available at LGH since April 2017, thanks to Ali’s advocacy efforts and a generous donation from the LGH Foundation Women’s Giving Circle.
FEES equipment allows SLPs such as Jana to directly visualize the upper airway while a patient is swallowing, to see what parts of the anatomy may not be working properly, what textures of food or drink are the safest, and to test the impact of positioning or other swallowing strategies and therapies on the patient’s swallow.
“Swallowing is a highly coordinated activity that is often taken for granted, but disordered swallowing – or dysphagia – is a common problem, particularly in an aging population,” explains Ali. “Being directly able to see what’s going on is an invaluable tool in reducing pneumonia rates, providing individualized education about swallowing, guiding swallowing therapies and preventing/minimizing hospital stays.”
Procedure requires in-depth academic + clinical training
For SLPs to perform this assessment, they are required to undergo in-depth academic and clinical training and must hold an Advanced Competency in FEES from the College of Speech and Hearing Health Professionals of BC. Certification is a long process, often taking a number of years to complete. Thanks to the presence of FEES equipment at LGH, Ali and Jana have been able to embark on this process, and will be the first SLPs at LGH to achieve this certification.
After the procedure is completed, Jana turns Mr. K’s chair to face the monitor so he can see what the camera recorded. As he watches, Jana explains to him what he is seeing, what might be the problem and how it can be corrected. In Mr. K’s case, Jana is able to observe inadequate airway protection on thin fluids – something she had suspected on bedside assessment, and is now able to definitively confirm. She is able to determine what components of his swallowing function are responsible for this – valuable information for guiding his swallowing rehabilitation. She is also able to offer Mr. K an immediate improvement in his diet, which may now include regular cut-up solid foods. The appointment with Mr. K takes just under an hour – set-up, procedure, education and review.
FEES helps inpatients & outpatients
To date, 18 patients, both inpatients and outpatients, have undergone FEES assessment at LGH, ranging in age from 47 to 94 years of age. These patients have trouble swallowing for a number of reasons, including stroke, head and neck cancer and Parkinsons.
“Sometimes the news is reassuring, and other times, cautionary,” says Ali. “Patients invariably leave with a better understanding of their body and its basic functioning – but in some cases, the information provided is literally lifesaving.”

Todd
Looks great. Do you work as part of a team with the ENT doctors and others? What happens when the patient has a vagal response or vomits and aspirates?
Fiona Hughes
Thanks for your questions, Todd. I will send them to SLP Ali Duke, who will be able to answer them for you.
Hi Todd. Here is Ali’s response:
Thanks for your response. We do not work as part of a team with ENTs at LGH, although we frequently communicate with ENTs in the course of our clinical work. We will often recommend ENT referral for our FEES patients, and ENTs will refer their patients to us for FEES. We rely on the referring doctor in addition to our own clinical judgement to screen patients for suitability to undergo endoscopy and take care with positioning of the scope, both on insertion and during feeding to avoid eliciting a gag. If any issues with patient tolerance present themselves, we are able to withdraw the scope immediately. In our acute care setting, both with our inpatients and outpatients, we have ready access to nurses, doctors and respiratory therapists, if needed. We have fortunately not encountered vagal responses or emesis in any of our patients to date.
Patricia
Good Work Ali and Team! The FEES (Fiberoptic Endoscopic Evaluation of Swallow) device is amazing! Congrats!