Team approach makes VGH Canadian leader in traumatic brain treatment
Just over a year ago Michael Severloh’s father got the call every parent dreads. “There has been an accident. It’s very serious. Your son has a traumatic brain injury.”
“My family didn’t know whether I would live or die,” says Michael. “Even if I did survive, they wondered what I would be like and how that would affect the rest of our lives.”
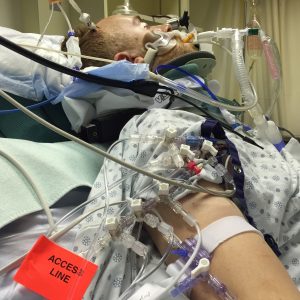
Patient Michael Severloh at VGH.
Michael had been hit by a car while cycling to school from his home in Kitsilano. The 30-year-old was rushed to Vancouver General Hospital where health care professionals from the critical care and neurosurgery teams placed Michael on life support and in a medically-induced coma.
According to VGH Intensivist Dr. Mypinder Sekhon, Michael had hemorrhages throughout his entire brain and brainstem, which controls the essential functions of consciousness. “Typically these types of injuries can result in death or a persistent vegetative state, with care eventually being withdrawn.”
Neurocritical care program at Vancouver General Hospital
VGH has recently developed a specialized neurocritical care program with a team consisting of a neurosurgeon, intensivist and ICU staff. “The approach to care has changed,” say Dr. Sekhon. “Our team and technology allows us to personalize care.” That team determined that Michael Severloh was a good candidate for advanced multimodal neuromonitoring, which allows physicians to individualize management decisions for each patient. Catheters were placed in Michael’s brain so his oxygen and blood pressure levels could be precisely monitored and optimized. “Michael’s oxygen levels were shockingly low, so we were able to boost his blood pressure, and in the ensuing days, his levels completely normalized,” says Dr. Sekhon.
Study shows positive patient outcomes
A study in the Canadian Journal of Neurological Sciences shows patients who underwent advanced neuromonitoring at VGH in the presence of a skilled neurocritical care team were 2.5 times more likely to have full neurological recovery after six months. The full PDF of the study is available here. The study tracked 113 patients with traumatic brain injuries admitted to the Intensive Care Unit (ICU) of VGH between February of 2010 and May 2016. The majority of the patients were young men and women, like Michael Severloh, who were injured in falls or motor vehicle accidents.
The results showed that with multimodal neuromonitoring, the favourable long term neurological outcome rate, which basically means people can live independently, increased from 37 percent to 60 percent. “This places VGH among the top reported outcome rates of leading international health centres including Cambridge in the U.K.” VGH is the only Canadian centre to report outcomes in this area.
“This is an example of what we do best at VGH.”
Dr. Marcel Dvorak, Associate Medical Director, VCH:
“This is an example of what we do best at VGH; taking care of the most critically ill and severely injured patients in the province of BC and providing them care that involves the highly sophisticated integration of multiple sub-specialists all focused on improving the health outcomes of our patients.”

Patient Michael Severloh, post treatment.
Michael Severloh credits the care he received at VGH for his remarkable recovery. “As it turns out, my brain is pretty resilient. Though therapies have helped in returning myself to me, mentally, I feel very similar to the way I was before the accident. But, ultimately, I have to credit my positive recovery to my bike helmet and the team at VGH.”


Kate
I’m so happy to see he had such a good recovery, I hope these advancements mean better outcomes for more patients. Will we be seeing this used routinely?
Sunny Oh
The VCH team has done 62 of these cases thus far. Whether this type of approach is appropriate is determined on a case-by-case basis, depending on the patient and the individual characteristics of the brain injury.